Sub-Saharan Africa : Infant Mortality Reduction Boasts Life Expectancy
- Par Kimeng Hilton
- 09 avril 2019 10:51
- 0 Likes
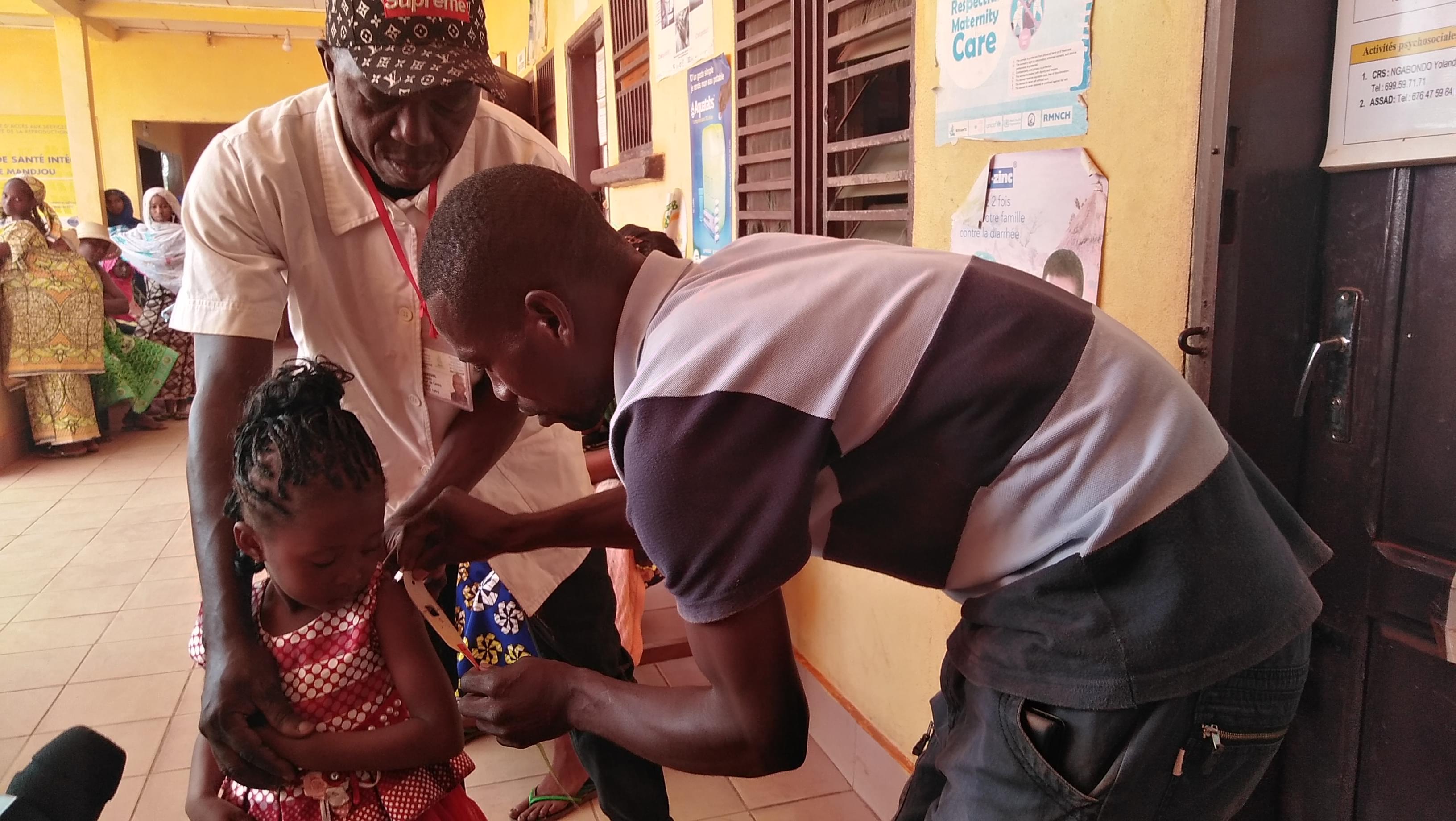
A report published by the World Health Organisation on April 7, 2019 says life expectancy has increased by five years since 2000.
Africa – especially Sub-Saharan Africa – tends to be associated with all forms of misery - related to disease, hunger, poverty … But this time around, there is some positive news from the continent and other developing countries. According to the 2019 World Health Statistics report published by the World Health Organisation, WHO, on the occasion of the World Heath Day on April 7, 2019, life expectancy in Sub-Saharan Africa increased by 5.5 years since 2000. This year’s report lays emphasis on primary healthcare as the foundation of universal health coverage.
“Life expectancy has increased largely thanks to reduction in mortality in children aged less than five years in poor countries. The number of deaths linked to measles dropped considerably. Likewise deaths associated with severe diarrhoea. On the other hand, deaths attributed to malaria dropped by half. Overall, infant mortality due to contagious diseases declined as life expectancy went up,” explained Dr. Richard Cibulskis, the main author of the study.
With this development, people can now expect to live to be 72 years on average. Between 2000 and 2016, global life-expectancy at birth increased by 5.5 years, from 66.5 to 72.0 years. Healthy life expectancy at birth - the number of years one can expect to live in full health - increased from 58.5 years in 2000 to 63.3 years in 2016. Life expectancy remains strongly affected by income. In low-income countries, it is 18.1 years lower than in high-income countries. One child in every 14 born in a low-income country will die before their fifth birthday, the report says.
“Breaking down data by age, sex and income group is vital for understanding who is being left behind and why,” said Dr Tedros Adhanom Ghebreyesus, WHO Director-General. “Behind every number in the World Health Statistics is a person, a family, a community or a nation. Our task is to use this data to make evidence-based policy decisions that move us closer to a healthier, safer, fairer world for everyone,” he added.
The gap between men’s and w...
Cet article complet est réservé aux abonnés
Déjà abonné ? Identifiez-vous >
Accédez en illimité à Cameroon Tribune Digital à partir de 26250 FCFA
Je M'abonne1 minute suffit pour vous abonner à Cameroon Tribune Digital !
- Votre numéro spécial cameroon-tribune en version numérique
- Des encarts
- Des appels d'offres exclusives
- D'avant-première (accès 24h avant la publication)
- Des éditions consultables sur tous supports (smartphone, tablettes, PC)














Commentaires